Anasazi and Wilderness Programs Outcomes
The Big Picture
Wilderness treatment (often referred to as Outdoor Behavioral Healthcare / OBH) is designed to help teens who are stuck in patterns like emotional shutdown, explosive conflict, defiance, school refusal, substance use, self-defeating choices, or high-risk peers. Across the research, wilderness/OBH outcomes most often fall into these buckets:

Overall emotional + behavioral functioning

Depression/ anxiety and other clinical symptom measures

Substance use, various addiction and relapse risk

Family relationships and communication

School adjustment / engagement
Evidence of Positive Outcomes in Wilderness Therapy
Research over the past two decades has consistently shown that wilderness therapy (also known as Outdoor Behavioral Healthcare, OBH) can lead to significant improvements in adolescents’ mental health and behavior. Multiple meta-analyses studies show that participants often enter these programs with clinical-level problems comparable to those in inpatient or residential treatment, yet by the end of a wilderness program many teens are functioning in the normal range of behavioral and emotional health. Below, we’ll review the research and outcomes behind wilderness and outdoor behavioral healthcare (OBH), and how these approaches compare with other treatment options.
Exploring the Impact of Wilderness Therapy: Evidence, Outcomes, and Ethics
What parents should know about wilderness treatment for struggling teens
When your teen is hurting (or acting in ways that scare you), it’s normal to want two things at the same time:

Real hope
something can help

Real proof
safe and works long-term.
This report is written for parents while grounding key points in the best available research.
Section 1:
Short-Term Outcomes with Wilderness Therapy
Research on Short-Term Outcomes with Wilderness Therapy
Wilderness treatment programs typically produce substantial short-term gains in teens’ emotional well-being, behavior, and life skills. By the conclusion of a program (often 6–12 weeks long), both youth and parent assessments show marked positive change. Some key improvements observed include:
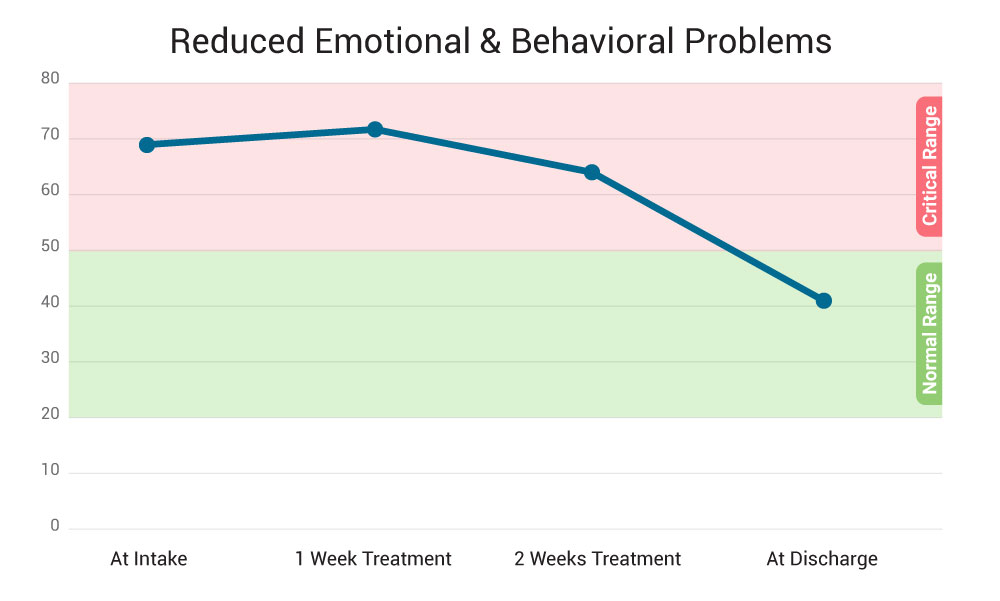
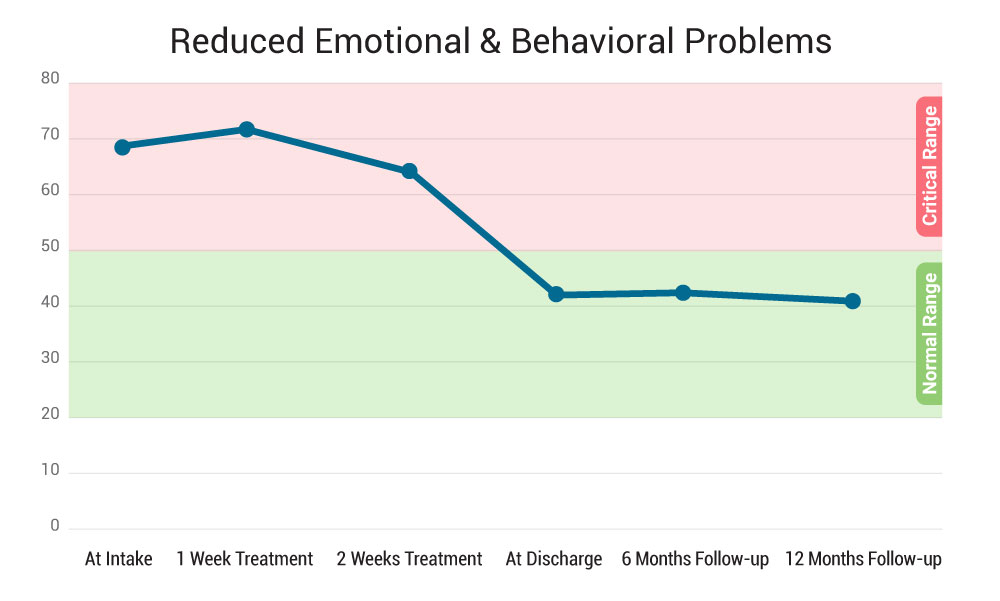
Reduced Emotional & Behavioral Problems
Teens report significantly fewer emotional struggles and behavioral issues at discharge from wilderness programs.
On a standard outcome questionnaire, youth move from a “clinical” level of dysfunction at intake to a “community” (normal) level of functioning by graduation.
For example, one program saw average youth symptom scores drop from about 69 (clinically distressed) at intake to ~41 (within normal range) upon completion – a change well above the threshold for meaningful improvement (based on outcome studies).
Source: Internal outcome data on youth completing wilderness therapy
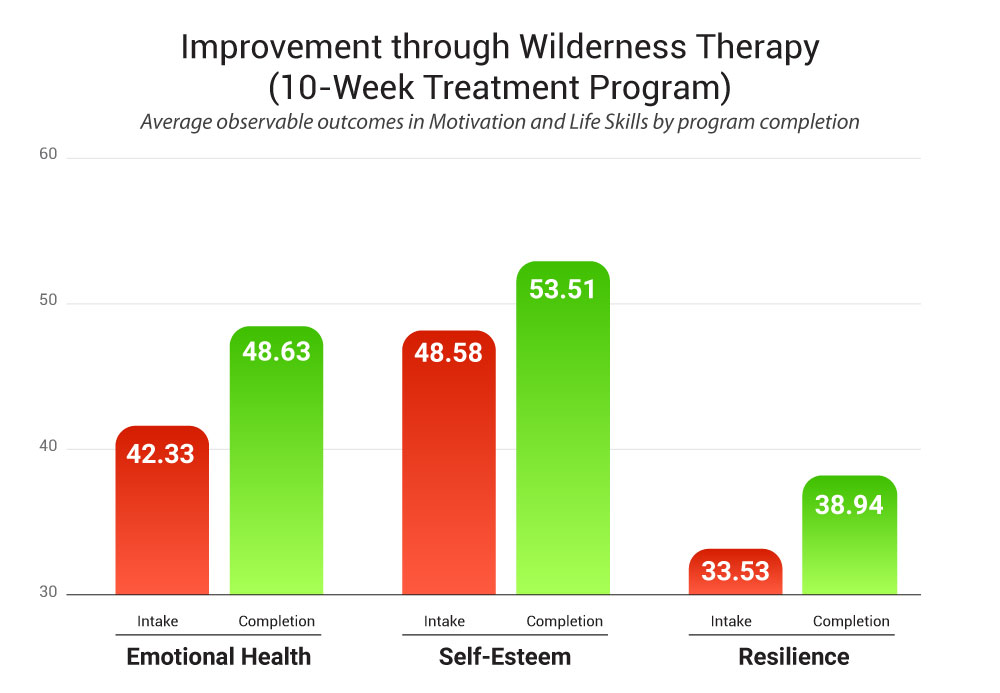
Improved Resilience and Confidence
Teens in the program showed growth in resilience and social self-esteem over the course of the wilderness experience. In simple terms, many left feeling more confident, more capable of handling challenges, and better able to manage difficult emotions. For teens who started the program with more serious struggles, the improvements were even stronger. These findings suggest that wilderness therapy can help teens build the inner strength and confidence they need to cope more effectively at home, at school, and in everyday life.
Source: Wilderness Adventure Therapy Effects on Mental Health of Youth
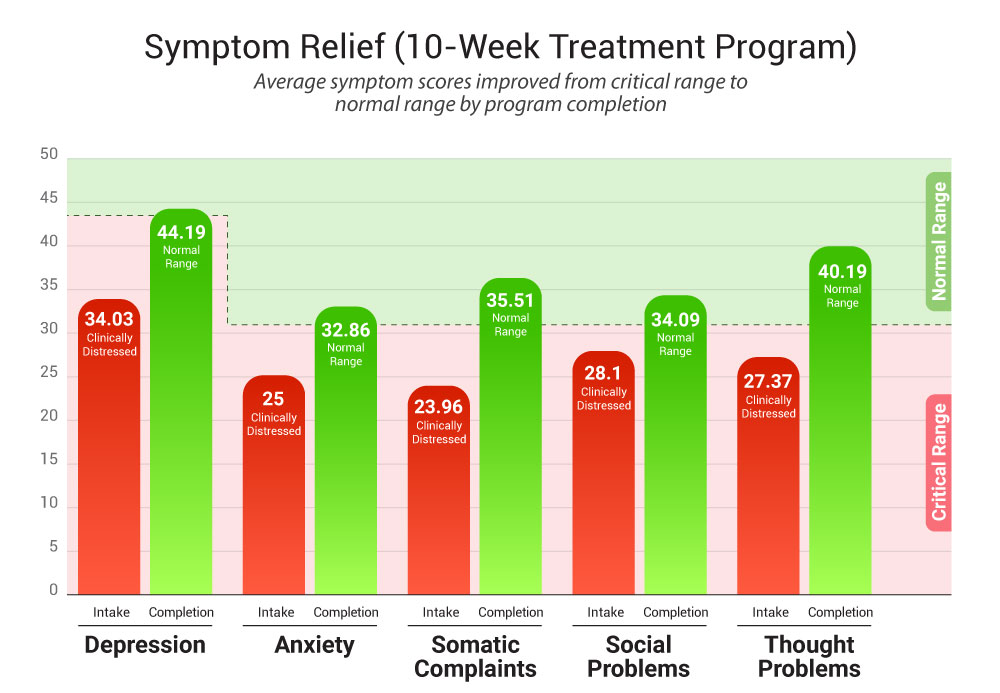
Symptom Relief
Clinical measures show reductions in depression, anxiety, and somatic complaints.
In one monitored group of at-risk adolescents, youth who started with severe clinical symptoms showed large drops in depression and big improvements in emotional/behavioral functioning by the end. These initial gains were comparable to those seen with regular therapy and indicated meaningful relief of acute symptoms.
Source: Wilderness Adventure Therapy Effects on Mental Health of Youth
Study: A Meta-Analysis of Outdoor Therapy Outcomes and Moderators
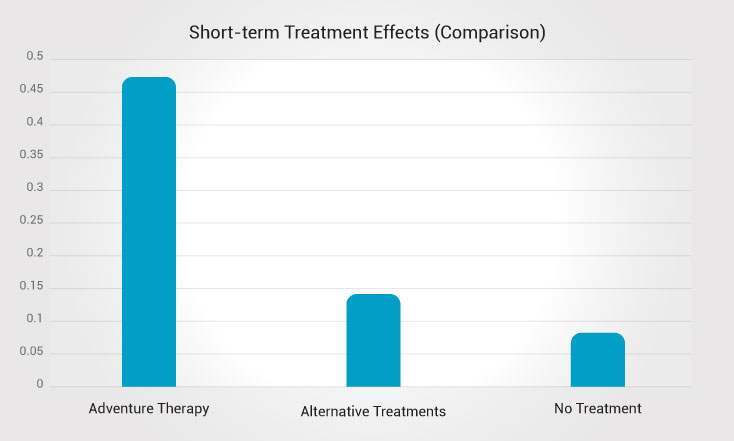
A major meta-analysis published in The Open Psychology Journal reviewed 197 studies of outdoor therapy (a broader category that overlaps with many wilderness and outdoor behavioral healthcare methods) and compared its short-term effects to those of other treatment options:
- Outdoor Therapy: g = 0.47
- Other alternative treatment: g = 0.14
- No treatment: g = 0.08
The analysis also found very little change during follow-up (g = 0.03), suggesting that outdoor therapy treatment gains were generally maintained over time.
Overall, the findings suggest teens often show meaningful improvement with outdoor therapy (3.4x higher compared to other alternative forms and 5.9x to no treatment), and many programs report that gains tend to hold – especially when families and aftercare supports are part of the plan.
Source: A meta-analysis of adventure therapy outcomes and moderators
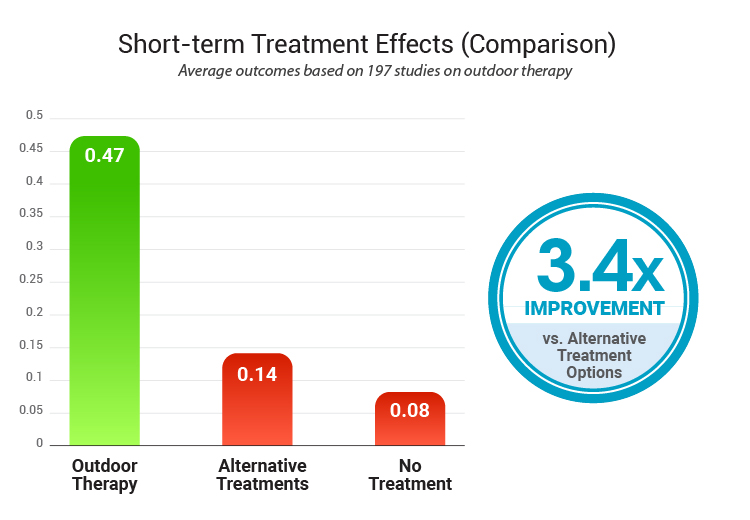
Note: Based on 197 studies on adventure therapy (over various short-term timelines)
Positive Outcomes Reported by Parents
Parents often corroborate these short-term results. In outcome tracking by one wilderness program, parents rated their teens as having far fewer behavioral problems and mood difficulties at discharge than before enrollment. Consistently, families observe their child leaving the wilderness program with greater maturity, resilience, and healthier family relationships than when they entered.
Source: Internal outcome data on youth completing wilderness therapy
Section 2:
Long-Term Outcomes / Benefits with Wilderness Therapy
Long-Term Wilderness / OBH Outcomes and Lasting Benefits
Critically, research suggests that the positive changes from wilderness therapy persist well after the program ends. Follow-up studies have tracked teens for months or years post-discharge and found maintained – even enhanced – improvements:
Maintained Progress
At 6 and 12 months after completing a wilderness program, graduates on average retain the gains they made in treatment.
For instance, one study found youth’s functional scores were ~40 at 6 and 12 months post-treatment (virtually unchanged from discharge and firmly in the normal range). While some mild resurgence of symptoms can occur, it is typically not clinically significant, and most teens remain far improved from their pre-treatment baseline.
In a program-level follow-up, clinicians noted that even 18 months later, alumni were overall still in a healthy range of functioning, indicating strong skill generalization to home life.
Source: Internal outcome data on youth completing wilderness therapy
One- to Two-Year Outcomes
Large-scale outcome research by the Outdoor Behavioral Healthcare Council examined hundreds of adolescents across multiple wilderness programs. They observed that initial clinical improvements were not only significant at discharge but were largely sustained one year later.
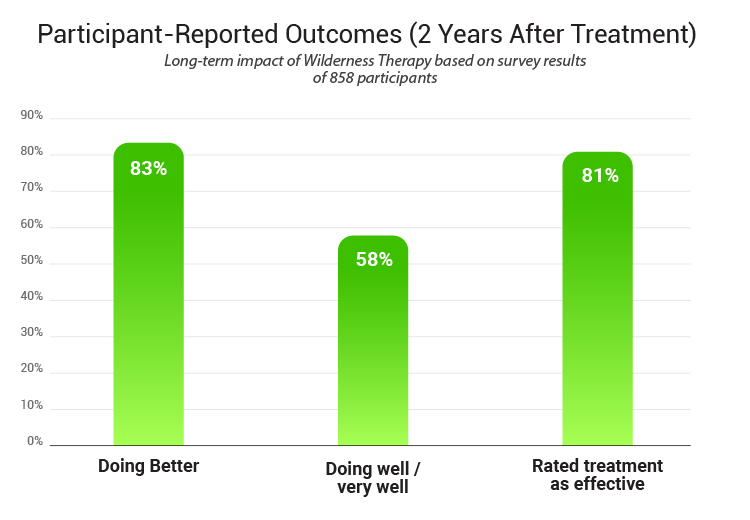
In interviews conducted two years after treatment, 83% of youths reported they were “doing better” than before, with 58% saying they were doing “well” or “very well”, and over 81% rating the wilderness therapy as an effective intervention in their lives. This indicates a strong long-term impact for the majority of participants.
Source: Internal outcome data on youth completing wilderness therapy
2 Year outcomes:
- 83% - Doing Better
- 58% - Doing Well or Very Well
- 80% - Rated as Effective Intervention
Lasting Symptom Reduction
A landmark study from the University of New Hampshire compared adolescents who completed an OBH wilderness program to a matched group who received traditional at-home therapy.
After 14 months, parents of the wilderness therapy teens reported their children were functioning significantly better than those who had only received usual treatments. In fact, at the one-year mark the Wilderness / OBH group showed almost three times the improvement in clinical symptom ratings compared to the non-wilderness group.
Importantly, these OBH teens maintained greater reductions in depression, anxiety, substance use, and other problem behaviors over the full year of follow-up.
Source: Internal outcome data on youth completing wilderness therapy
1 Year outcomes:
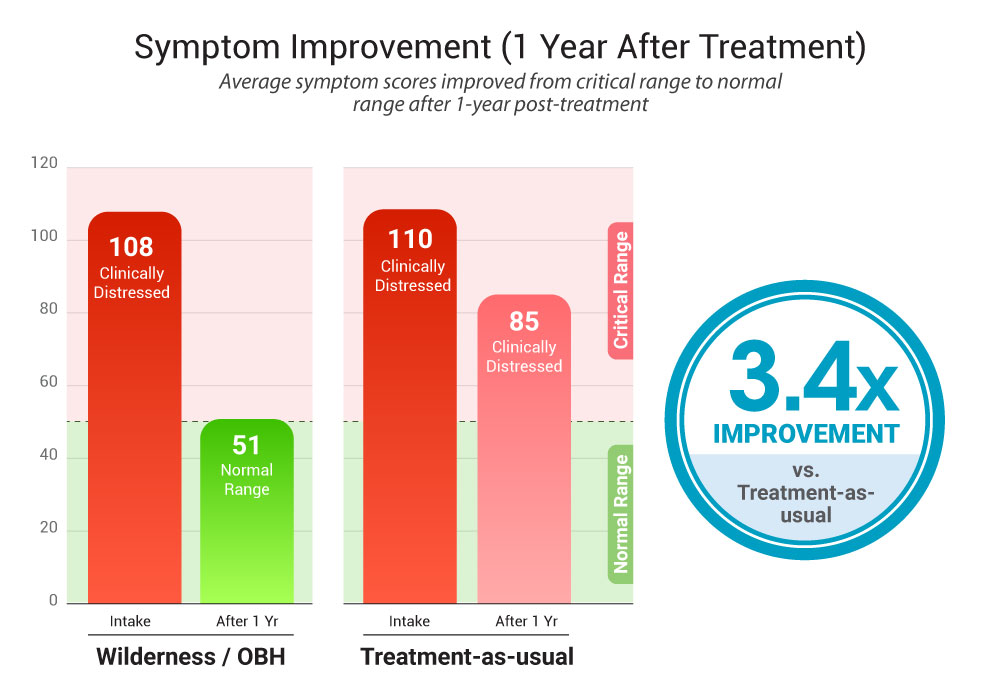
Note: Lower scores indicate improvement over time.
Study: A Meta-Analysis of Adventure Therapy Outcomes and Moderators
A major meta-analysis published in The Open Psychology Journal reviewed 197 studies of adventure therapy (a broader category that overlaps with many wilderness and outdoor behavioral healthcare methods) and compared its short-term effects to those of other treatment options:
- Adventure Therapy: g = 0.47
- Other alternative treatment: g = 0.14
- No treatment: g = 0.08
The analysis also found very little change during follow-up (g = 0.03), suggesting that adventure therapy treatment gains were generally maintained over time.
Overall, the findings suggest teens often show meaningful improvement with adventure therapy (3.4x higher compared to other alternative forms and 5.9x to no treatment), and many programs report that gains tend to hold – especially when families and aftercare supports are part of the plan.
Source: A meta-analysis of adventure therapy outcomes and moderators
A Foundation for Lasting Change
Overall, the evidence points to wilderness therapy providing not just a “quick fix,” but enduring benefits for many troubled teens. By imparting coping skills, self-efficacy, and healthier family dynamics, these programs help set youth on a more positive trajectory that continues long after they return from the wilderness.
Section 3:
Anasazi Outcomes (15-Year Case Study)
Anasazi Participant Outcomes: A 15-Year Case Study
(Anasazi Evaluation Report)
This report tracks participant outcomes from intake through discharge over the past 15 years, using standardized questionnaires as well as satisfaction surveys from parents/caregivers and participants.
Across this period, parents overwhelmingly reported that the program helps, and the measured scores show large improvements by discharge, with meaningful progress present after the program. These findings suggest meaningful progress during treatment and provide important insight into the question: Does it work?
Important note: Participant outcomes can vary based on individual circumstances, challenges, and environment.
Study Snapshot
- Study Duration: 2011-2025 (15 years)
- Participants: 1,876
- Ave Length of Stay: 49.5 days
- Ave Age: 16-18
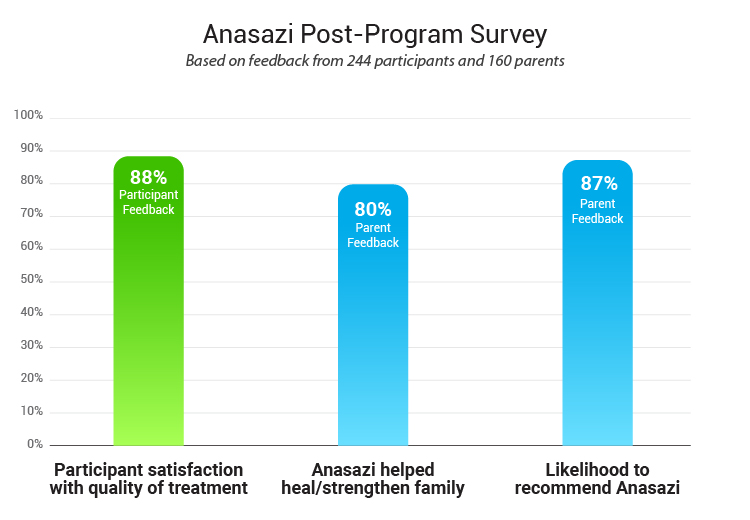
Anasazi Post-program parent survey
- Likelihood to recommend Anasazi:
- Anasazi helped heal/strengthen the family:
- Participant satisfaction with quality of treatment:
Anasazi received consistently strong marks from both parents and participants.
Among 106 parent respondents, the average likelihood to recommend the program was 6.1 out of 7, and parents rated Anasazi’s role in healing and strengthening their family at 5.4 out of 6.
Participants also rated the quality of treatment highly, with an average score of 4.4 out of 5 at discharge (n = 244) and the same 4.4 out of 5 post-discharge (n = 177), indicating that these positive perceptions continued beyond the program itself.
Anasazi Parent-Reported Improvements
The evaluation uses standardized scales where higher scores indicate more distress/strain/dysfunction, so lower scores = improvement.
1) Emotional distress (parent/caregiver ratings)
- At intake: ~33–35 (clinical range)
- At discharge:: ~6–12 (healthy range)
Summary: Parents saw distress drop dramatically by discharge, and while some “rebound” can happen after returning home, the average remained meaningfully better than where families started.
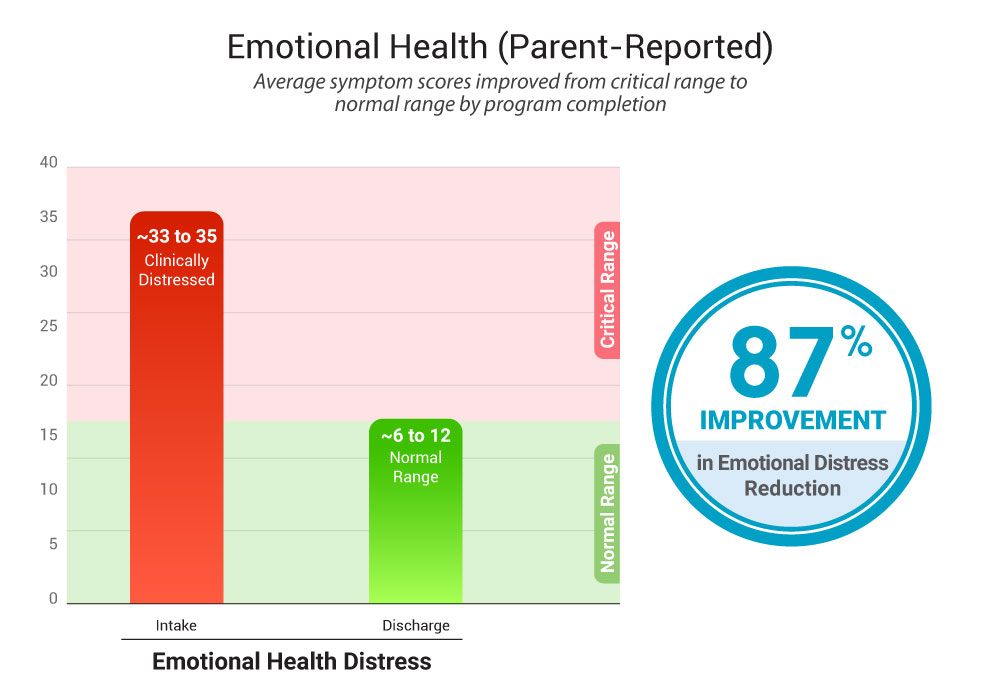
Note: Lower scores indicate improvement over time.
2) Parent-teen relationship strain
- At intake: ~14.6–14.8 (distressed range)
- At discharge:: ~0.2–3.4 (healthy range)
Summary: One of the strongest “family story” statistics is that relationship strain improved from the “distressed” range to the “healthy” range during the program and remained meaningfully improved afterward.
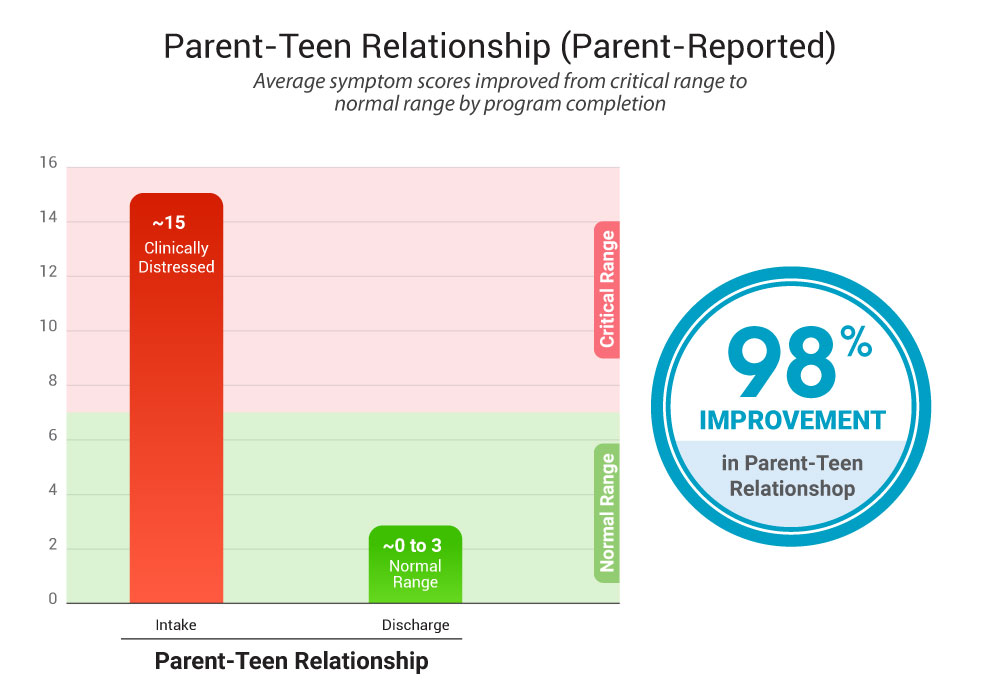
Note: Lower scores indicate improvement over time.
3) Behavior dysfunction (parent/caregiver ratings)
- At intake: 21–22
- At discharge:: ~4–9 (healthy range)
Parent and caregiver ratings showed substantial improvement in behavioral functioning from intake to discharge. This suggests a marked reduction in behavioral dysfunction over the course of treatment.
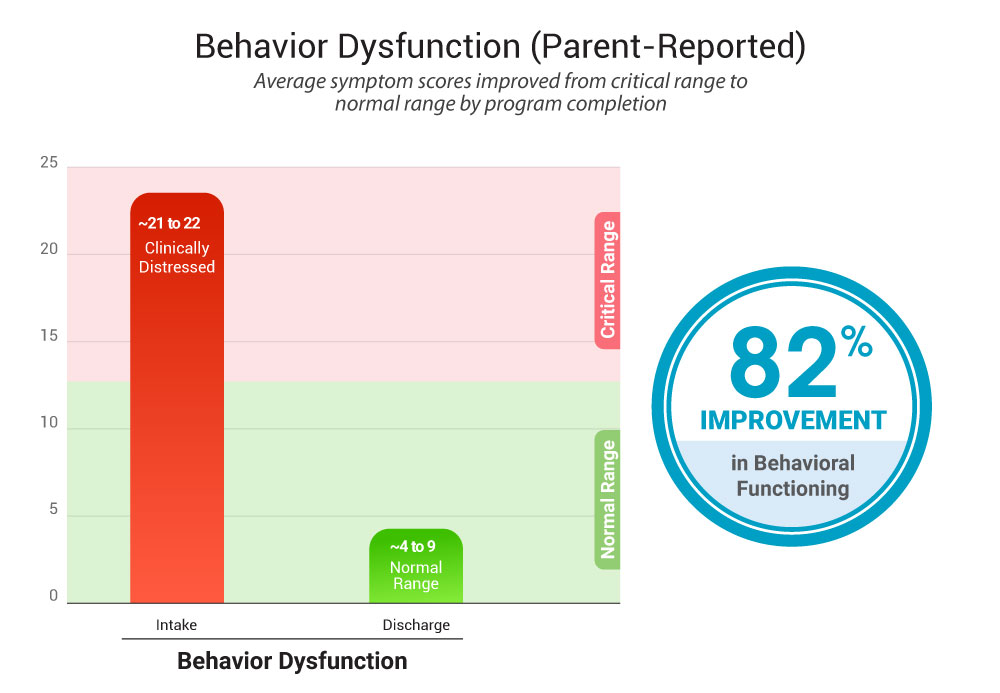
Note: Lower scores indicate improvement over time.
4) Overall functioning (parent/caregiver total score)
- At intake: ~99–102
- At discharge:: ~16–36 (healthy range)
Summary: “Across the big-picture ‘overall functioning’ score, families typically see the biggest improvement by discharge.
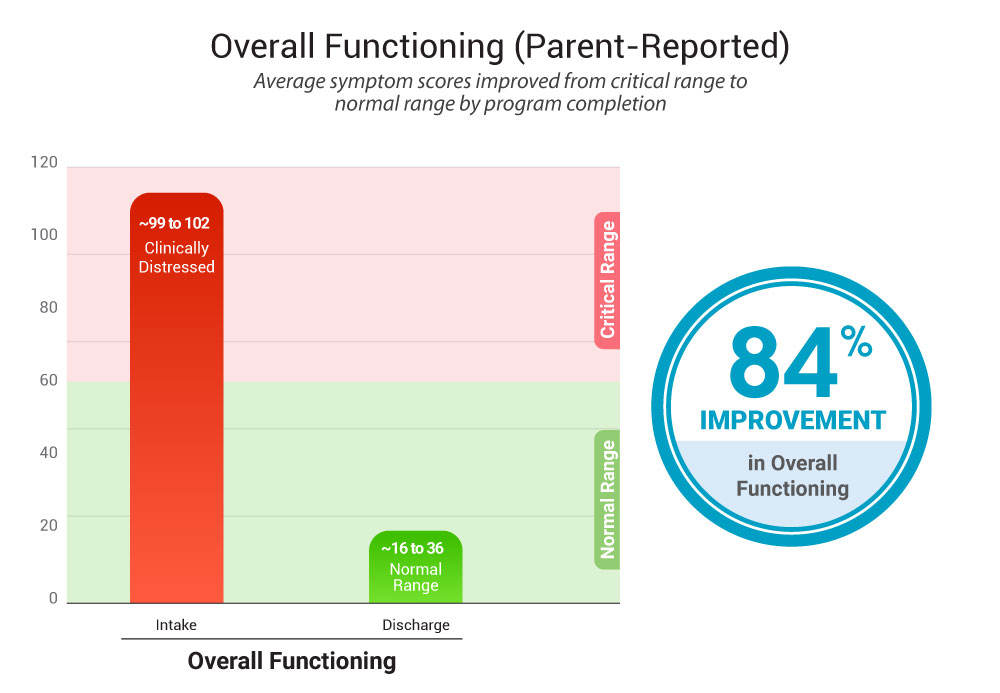
Note: Lower scores indicate improvement over time.
5) Safety snapshot
Across 38 years (1988-2026):
- 124,886 client-days
- 0 fatalities or catastrophic injuries

Section 4:
Wilderness Therapy vs Traditional Treatments
Comparing Wilderness Therapy to Traditional Treatments
One question parents often ask is how wilderness therapy outcomes stack up against more conventional treatment options (such as weekly counseling, outpatient programs, or inpatient care). Research indicates that wilderness programs can meet or exceed the effectiveness of traditional therapies, especially in achieving lasting change:
Higher Success and Completion Rates
Wilderness therapy engages teens in a novel, immersive way that often leads to better adherence.
In one analysis of adolescents with substance abuse and mental health comorbidities, 94% of youth completed the outdoor treatment program, versus only 37% completion in a comparable “treatment-as-usual” setting.
This high engagement means more teens actually finish treatment and reap its full benefits, whereas many drop out of standard programs.
94% of youth completed the outdoor treatment program, versus only 37% completion compared to standard treatment (pmc.ncbi.nlm.nih.gov)
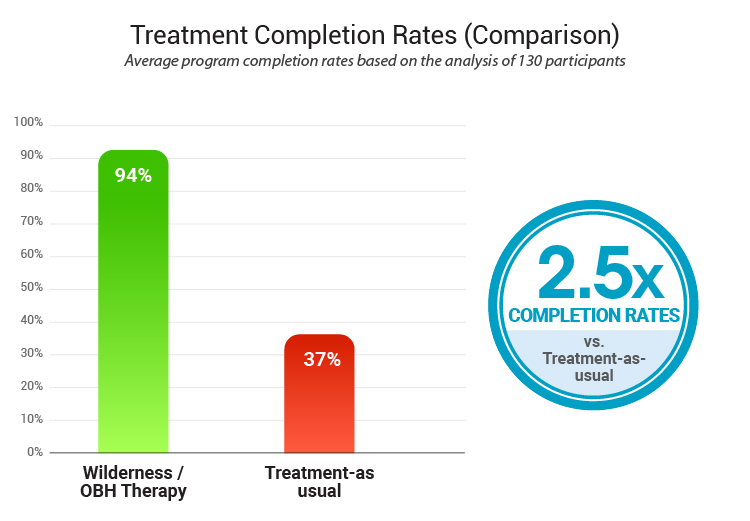
Note: Higher scores indicate improvement over time.
Greater Clinical Improvement
The same study found dramatically larger gains for the wilderness group.
Using a standardized behavioral health outcome measure, the Wilderness / OBH participants showed 424% greater improvement than those in regular treatment. In practical terms, the wilderness therapy teens had far bigger reductions in symptom severity and problem behaviors.
Similarly, the UNH comparison study described earlier found Wilderness / OBH participants had roughly 3x the symptom improvement of peers who stayed home in outpatient therapy after one year.
These findings suggest that for many struggling adolescents, the intensive wilderness approach can produce deeper healing and personal growth than traditional therapy alone.
The Value of Outdoor Behavioral Healthcare
Wilderness / OBH participants showed 424% greater improvement than those in regular treatment. (pmc.ncbi.nlm.nih.gov)
Wilderness / OBH participants had roughly 3× the symptom improvement of peers who stayed home in outpatient therapy after one year. (UNH Research)
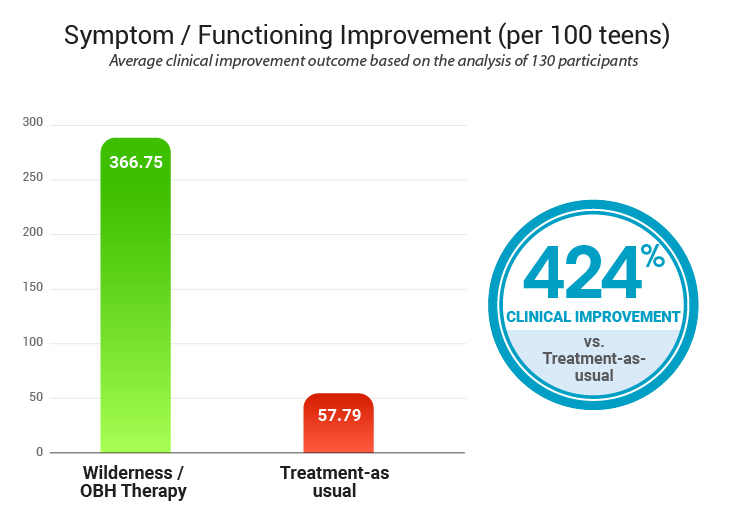
Note: Higher scores indicate improvement over time.
Lasting Impact
A notable strength of wilderness programs is how well teens retain their progress. Conventional treatments may show gains initially, but relapse rates can be high.
By contrast, outdoor behavioral healthcare has demonstrated longer-lasting effects. Researchers attribute this to the immersive, experiential learning model – teens practice new skills in real time and build confidence through overcoming wilderness challenges, making the lessons “stick” better once they return home.
In the UNH study, wilderness therapy youths not only improved more during treatment, but maintained those improvements longer than youths in standard care.
Source: University of New Hampshire (UNH) Research
Wilderness / OBH showed Longer lasting effects over standard treatments (UNH Research)
Note: Lower scores indicate improvement over time.
Cost-Effectiveness
Source: The Value of Outdoor Behavioral Healthcare
Wilderness / OBH had 60% higher cost-benefit ratio than standard treatment-as-usual
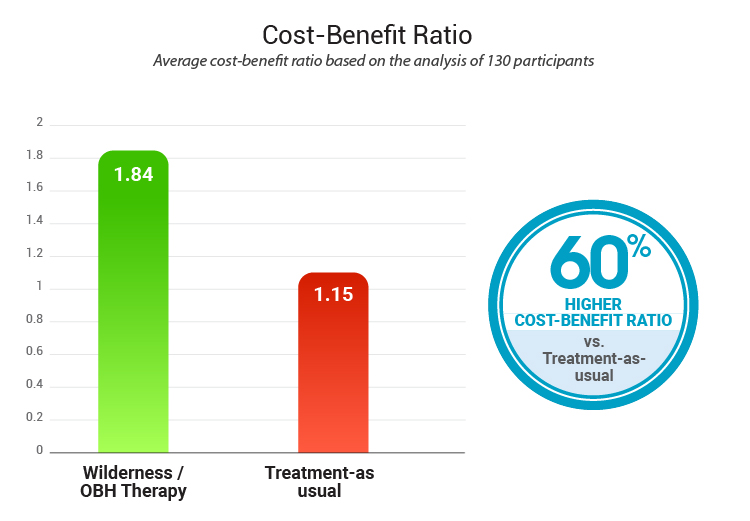
Note: Higher scores indicate better cost-benefit ratio.
Study: The effectiveness of outdoor behavioral healthcare with struggling adolescents
A study published in Children and Youth Services Review looked at teens in wilderness/outdoor behavioral healthcare (OBH) and compared them with teens receiving standard community treatment.
Starting point
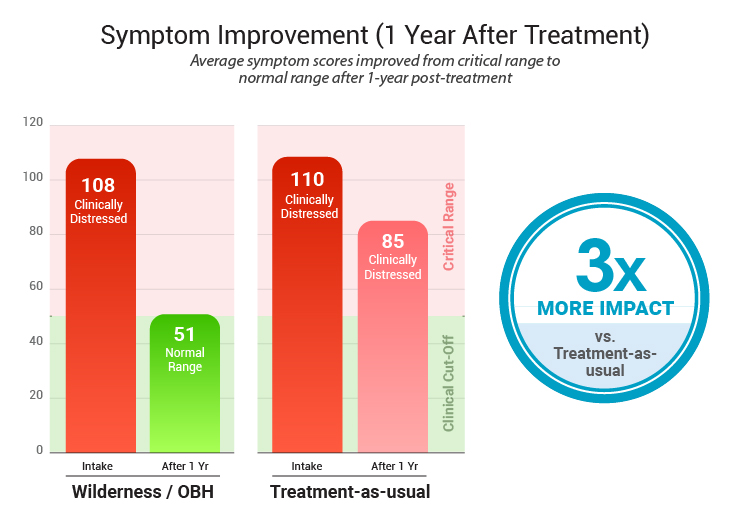
- Wilderness/OBH: 107.23
- Standard treatment: 106.87
About one year later
- Wilderness/OBH: 51.53 (55.7 difference)
- Standard treatment: 86.92 (19.95 difference)
Lasting Impact
A notable strength of wilderness programs is how well teens retain their progress. Conventional treatments may show gains initially, but relapse rates can be high.
By contrast, outdoor behavioral healthcare has demonstrated longer-lasting effects. Researchers attribute this to the immersive, experiential learning model – teens practice new skills in real time and build confidence through overcoming wilderness challenges, making the lessons “stick” better once they return home.
In the UNH study, wilderness therapy youths not only improved more during treatment, but maintained those improvements longer than youths in standard care.
Source: University of New Hampshire (UNH) Research
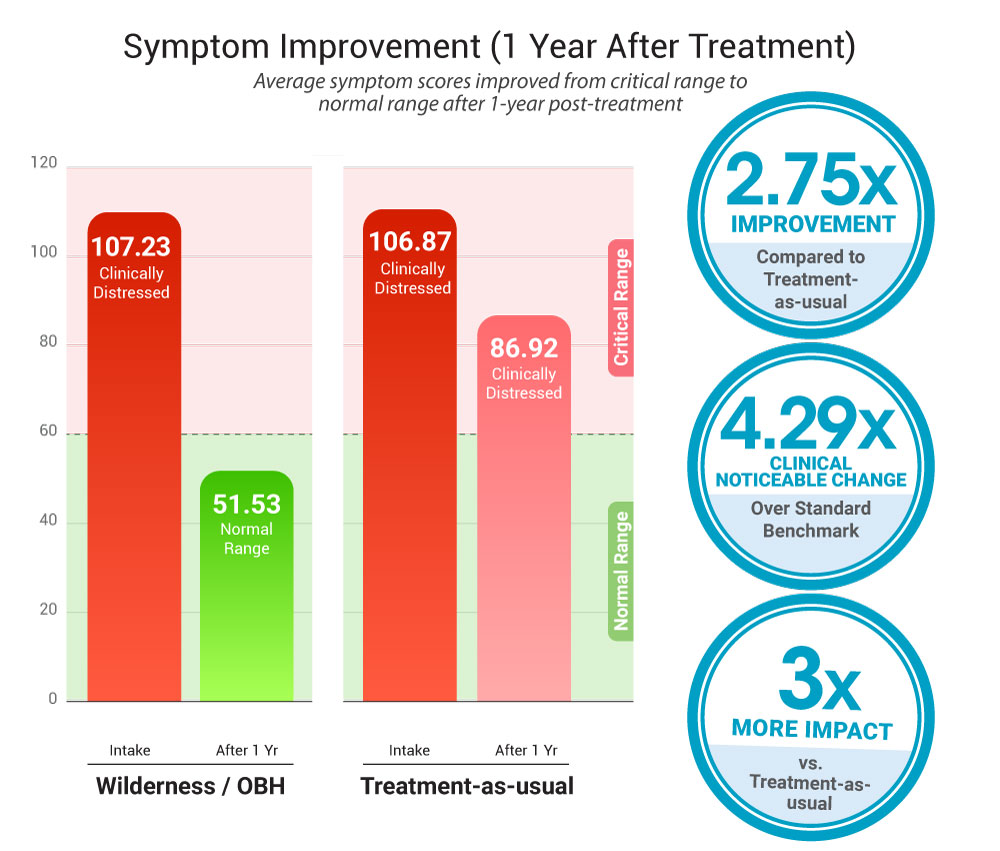
Note: Lower scores indicate improvement over time.
Why this matters
At the beginning of the study, both groups were struggling at about the same level with scores well above the clinical cutoff of 47, meaning both groups started with serious emotional and behavioral challenges.
At follow-up, the wilderness therapy group showed much greater improvement with a 55.7 points improvement from their starting score. By comparison, teens in standard treatment improved by 19.95 points from baseline. This means the wilderness therapy group showed substantially greater improvement overall – about 3x more than the standard treatment group.
Over the course of about a year, families reported major gains in teens who participated in wilderness therapy. Teens in standard treatment also improved, but on average they continued to show more significant ongoing difficulties at follow-up.
Source: The effectiveness of outdoor behavioral healthcare
A Promising Option
It’s important to note that every teen is unique, and some may respond differently to various interventions. However, the growing body of research makes it clear that reputable wilderness therapy programs are highly effective for many adolescents – often matching or outperforming traditional therapeutic approaches on key outcomes. For parents exploring treatment options, this suggests that wilderness therapy may be a credible, evidence-supported path toward meaningful emotional and behavioral progress.
Section 5:
Safety and Ethics: What Responsible Programs Do Differently
Safety and ethics: what responsible programs do differently
Unfortunately, the broader “troubled teen” space has included unethical private residential programs and related services that have caused real harm. Those failures have understandably damaged public trust—and, in the process, unfairly cast a shadow over accredited, ethical providers who are genuinely helping teens and families make meaningful progress.
Not all programs are the same – What parents should look for
Independent standards/accreditation: The Association for Experiential Education (AEE) describes an Wilderness / OBH accreditation framework that includes ethical standards, risk management, and treatment standards for the field.
A parent-friendly “Safety Checklist”
A program should be fully Accredited and willing to explain (clearly, without defensiveness):
- Who provides clinical care and what credentials they hold
- How medical screening and medication management are handled
- Staff training, supervision, ratios, and emergency procedures
- How incidents are documented and reviewed
- How parents are included (family therapy, calls, progress updates)
- What transition and aftercare planning looks like
Wilderness Therapy Safety in Perspective
While no program can promise complete safety for every adolescent, research suggests that teens in Wilderness / OBH programs may face lower overall risk than teens who are not in these programs.
In 2012, the average U.S. adolescent was about twice as likely to visit an emergency room as an Wilderness / OBH participant. Injury rates reported by OBH Council programs are also substantially lower than many everyday activities teens commonly do.
For example, injuries during high school football games are reported to be more than 328 times as common as injuries in OBH Council outdoor therapy programs. Even compared with a more similar activity, teen backpacking is reported to be about 20 times more likely to result in injury than comparable activities within an OBH Council program.
Source: Adventure therapy: Theory, research, and practice

Conclusion
Wilderness therapy often immerses teens in challenging outdoor experiences under the guidance of therapists. This experiential approach helps build confidence, resilience, and healthy coping skills in troubled teens. Research indicates that such programs not only reduce problem behaviors in the short term, but also foster personal growth that endures long after the wilderness journey.
For parents considering a wilderness treatment program like the Anasazi Foundation for their teen, the evidence is encouraging. Short-term outcome studies show significant reductions in teens’ depression, anxiety, defiance, and substance use, alongside improvements in self-esteem and family relationships. Long-term research further demonstrates that these positive changes are largely sustained – graduates often continue to do well a year or two down the road, applying the skills and self-confidence gained in the wilderness to their daily lives. Moreover, when compared to other interventions, wilderness therapy has been shown to hold its own or even outshine traditional treatments on measures of clinical improvement and lasting impact. All told, reputable wilderness therapy programs offer a promising, evidence-backed option for struggling teens, providing healing in the short term and hope for the long term.
Sources
- DeMille, S. et al. (2018). The effectiveness of outdoor behavioral healthcare with struggling adolescents: A comparison group study. Children and Youth Services Review.
- Wilson, S. J., & Lipsey, M. W. (2000). Wilderness challenge programs for delinquent youth: A meta-analysis
- Bowen, D. J., & Neill, J. T. (2013). A meta-analysis of adventure therapy outcomes and moderators. The Open Psychology Journal.
- Washington State Institute for Public Policy (WSIPP) (2022). Wilderness Therapy Programs: A Systematic Review of Research.
- CrimeSolutions.gov (U.S. DOJ) (2019). Wilderness Challenge Programs (Rated Practice).
- 6. U.S. Government Accountability Office (GAO) (2008). Residential Programs: Selected Cases of Death, Abuse, and Deceptive Marketing (GAO-08-713T).
- Association for Experiential Education (AEE). Manual for Accreditation for OBH Programs / AEE Accreditation.
- Utah Legislature (2025). H.B. 491 definition of “Outdoor youth program” (includes wilderness therapy / OBH).
- Russell, K. et al. “Outcomes in Outdoor Behavioral Healthcare: 2-Year Follow-Up Results.” OBH Council Research, via Second Nature .
- Gass, M. et al. “The Value of Outdoor Behavioral Healthcare for Adolescent Substance Users with Comorbid Conditions.” SAGE Open (2019): Cost-effectiveness and outcomes comparison of OBH vs. traditional treatment.
- Bowen, D. et al. “Wilderness Adventure Therapy Effects on Mental Health of Youth.” Eval. and Program Planning 58 (2016): 49–59. (WAT program study in Australia – WAT as effective as traditional therapy for symptomatic youth).
- Second Nature Therapy Programs – Outcome Studies. Internal outcome data on youth completing wilderness therapy (YOQ score changes, functional improvements, follow-up maintenance).
- University of New Hampshire (UNH) Research (2018) – Press Release on a comparison study of OBH vs. outpatient therapy, showing greater and longer-lasting improvement in the wilderness group.
- Gass, M. A., Gillis, H. L. “L.”, & Russell, K. C. (2012). “Adventure therapy: Theory, research, and practice.” Routledge/Taylor & Francis Group.